Abstract
Diabetic wound management is a serious health care challenge due to higher rates of relapse, expensive treatment approaches, and poor healing outcomes. Among cell-based therapies, use of platelet-rich plasma (PRP) has been shown to be effective for diabetic wounds, but its poor shelf-life limits its clinical use. Here, we demonstrate a simple but effective polymer system to increase the shelf-life of PRP by developing a polyelectrolyte complex with dropwise addition of chitosan solution containing PRP by simple mixing at room temperature. Thus, prepared chitosan-fucoidan (CF) carrier complex encapsulated more than 95% of the loaded PRP. The resulting CF/PRP colloids were spherical in shape and ensured extended PRP release up to 72 h at 37 °C. Routine characterization (FT-IR, XRD, SEM) showed the material properties. The biological assays showed that CF complexes were biocompatible while CF/PRP enhanced the proliferation of fibroblasts and keratinocytes via higher Ki67 expression and fibroblast migration. Further investigations using a diabetic mouse model demonstrated significantly higher wound contraction and histopathological observations showed increased fibroblast migration, and collagen and cytokeratin deposition in treatment groups. The results are suggestive of the efficacy of CF/PRP as a cost-effective topical formulation for the sustained delivery of growth factors in treating chronic diabetic wounds.
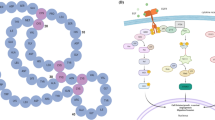
Graphical abstract












Similar content being viewed by others
Availability of data and materials
All data related to the study are within the manuscript.
References
Patel S, Srivastava S, Singh MR, Singh D. Mechanistic insight into diabetic wounds: pathogenesis, molecular targets and treatment strategies to pace wound healing. Biomed Pharmacother. 2019;112:108615.
Baltzis D, Eleftheriadou I, Veves A. Pathogenesis and treatment of impaired wound healing in diabetes mellitus: new insights. Adv Ther. 2014;31(8):817–36.
Barrientos S, Brem H, Stojadinovic O. Clinical application of growth factors and cytokines in wound healing. Wound Repair Regen. 2014;22(5):569–78.
Wahbi AA. Auto amputation of diabetic toe with dry gangrene: a myth or a fact? Diabetes Metab Syndr Obes. 2018;11:255–64.
Heuch L, Gomersall JS. Effectiveness of offloading methods in preventing primary diabetic foot ulcers in adults with diabetes: a systematic review. JBI evid synth. 2016;14(7):236–65.
Hemsinli D, Altun G, Kaplan ST, Yildirim F, Cebi G. Hyperbaric oxygen treatment in thromboangiitis obliterans: a retrospective clinical audit. Diving Hyperb Med. 2018;48(1):31–5.
Rekha PD, Rao SS, Sahana TG, Prabhu A. Diabetic wound management. Br J Community Nurs. 2018;23(9):16–22.
Hinderer S, Layland SL, Schenke-Layland K. ECM and ECM-like materials—biomaterials for applications in regenerative medicine and cancer therapy. Adv Drug Deliv Rev. 2016;97:260–9.
Dawood AS, Salem HA. Current clinical applications of platelet-rich plasma in various gynecological disorders: an appraisal of theory and practice. Clin Exp Reprod Med. 2018;45(2):67–74.
Chellini F, Tani A, Zecchi-Orlandini S, Sassoli C. Influence of platelet-rich and platelet-poor plasma on endogenous mechanisms of skeletal muscle repair/regeneration. Int J Mol Sci. 2019;20(3):683.
Etulain J. Platelets in wound healing and regenerative medicine. Platelets. 2018;29(6):556–68.
Hussain N, Johal H, Bhandari M. An evidence-based evaluation on the use of platelet rich plasma in orthopedics - a review of the literature. SICOT-J. 2017;3.
Pino-Sedeño TD, Trujillo-Martín MM, Andia I, Aragón-Sánchez J, Herrera-Ramos E, Iruzubieta Barragán FJ, Serrano-Aguilar P. Platelet-rich plasma for the treatment of diabetic foot ulcers: a meta-analysis. Wound Repair Regen. 2019;27(2):170–82.
Hu Z, Qu S, Zhang J, Cao X, Wang P, Huang S, Shi F, Dong Y, Wu J, Tang B, Zhu J. Efficacy and safety of platelet-rich plasma for patients with diabetic ulcers: a systematic review and meta-analysis. Adv Wound Care. 2019;8(7):298–308.
Rao SS, Venkatesan J, Prabhu A, Rekha PD. Natural polymeric biomaterials in growth factor delivery for treating diabetic foot ulcers. J Drug Deliv Sci Technol. 2020;55:101385.
Hoare TR, Kohane DS. Hydrogels in drug delivery: progress and challenges. Polymer. 2008;49(8):1993–2007.
Ghasemiyeh P, Mohammadi-Samani S. Hydrogels as drug delivery systems; pros and cons. Trends Pharmacol Sci. 2019;5(1):7–24.
Barclay TG, Day CM, Petrovsky N, Garg S. Review of polysaccharide particle-based functional drug delivery. Carbohydr Polym. 2019;221:94–112.
Lankalapalli S, Kolapalli VR. Polyelectrolyte complexes: a review of their applicability in drug delivery technology. Indian J Pharm Sci. 2009;71(5):481.
Oliveira C, Neves NM, Reis RL, Martins A, Silva TH. Gemcitabine delivered by fucoidan/chitosan nanoparticles presents increased toxicity over human breast cancer cells. Nanomedicine. 2018;13(16):2037–50.
Lu KY, Li R, Hsu CH, Lin CW, Chou SC, Tsai ML, Mi FL. Development of a new type of multifunctional fucoidan-based nanoparticles for anticancer drug delivery. Carbohydr Polym. 2017;165:410–20.
Huang YC, Yang YT. Effect of basic fibroblast growth factor released from chitosan–fucoidan nanoparticles on neurite extension. J Tissue Eng Regen Med. 2016;10(5):418–27.
Barbosa AI, Lima SAC, Reis S. Application of pH-responsive fucoidan/chitosan nanoparticles to improve oral quercetin delivery. Molecules. 2019;24(2):346.
Huang YC, Li RY. Preparation and characterization of antioxidant nanoparticles composed of chitosan and fucoidan for antibiotics delivery. Mar Drugs. 2014;12(8):4379–98.
Sahana TG, Rekha PD. Biopolymers: applications in wound healing and skin tissue engineering. Mol Biol Rep. 2018;45(6):2857–67.
Zeng HY, Huang YC. Basic fibroblast growth factor released from fucoidan-modified chitosan/alginate scaffolds for promoting fibroblasts migration. J Polym Res. 2018;25(3):1–9.
Kumaran MS. Platelet-rich plasma in dermatology: boon or a bane? Indian J Dermatol Venereol Leprol. 2014;80(1):5–14.
Amable PR, Carias RB, Teixeira MV, Pacheco ÍDC, Amaral RJD, Granjeiro JM, Borojevic R. Platelet-rich plasma preparation for regenerative medicine: optimization and quantification of cytokines and growth factors. Stem Cell Res Ther. 2013;4(3):1–3.
Bradford MM. A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal Biochem. 1976;72(1–2):248–54.
Mosmann T. Rapid colorimetric assay for cellular growth and survival: application to proliferation and cytotoxicity assays. J Immunol Methods. 1983;65(1–2):55–63.
Yarrow JC, Perlman ZE, Westwood NJ, Mitchison TJ. A high-throughput cell migration assay using scratch wound healing, a comparison of image-based readout methods. BMC Biotechnol. 2004;4(1):1–9.
Bose B, Shenoy SP, Konda S, Wangikar P. Human embryonic stem cell differentiation into insulin secreting β-cells for diabetes. Cell Biol Int. 2012;36(11):1013–20.
Park HB, Yang JH, Chung KH. Characterization of the cytokine profile of platelet rich plasma (PRP) and PRP-induced cell proliferation and migration: upregulation of matrix metalloproteinase-1 and-9 in HaCaT cells. Korean J Hematol. 2011;46(4):265–73.
Chicharro-Alcántara D, Rubio-Zaragoza M, Damiá-Giménez E, Carrillo-Poveda JM, Cuervo-Serrato B, Peláez-Gorrea P, Sopena-Juncosa JJ. Platelet rich plasma: new insights for cutaneous wound healing management. J Funct Biomater. 2018;9(1):10.
Downing SR, Klement GL. Isolation and proteomic analysis of platelets by SELDI-TOF MS. InSELDI-TOF Mass Spectrometry. Springer, New York, NY. 2012;153–170.
Huang YC, Kuo TH. O-Carboxymethyl chitosan/fucoidan nanoparticles increase cellular curcumin uptake. Food Hydrocoll. 2016;53:261–9.
Coutinho AJ, Lima SA, Afonso CM, Reis S. Mucoadhesive and pH responsive fucoidan-chitosan nanoparticles for the oral delivery of methotrexate. Int J Biol Macromol. 2020;158:180–8.
Stoscheck CM. Quantitation of protein. Meth Enzymol. 1990;182:50–68.
Julkapli NM, Ahmad Z, Akil HM. Preparation and characterization of 1, 2, 4, 5-benzenetetra carboxylic-chitosan. e-Polymers. 2010;10(1).
Lee MC, Huang YC. Soluble eggshell membrane protein-loaded chitosan/fucoidan nanoparticles for treatment of defective intestinal epithelial cells. Int J Biol Macromol. 2019;131:949–58.
Sah MK, Pramanik K. Soluble-eggshell-membrane-protein-modified porous silk fibroin scaffolds with enhanced cell adhesion and proliferation properties. J Appl Polym Sci. 2014;131(8):40138.
Wu SJ, Don TM, Lin CW, Mi FL. Delivery of berberine using chitosan/fucoidan-taurine conjugate nanoparticles for treatment of defective intestinal epithelial tight junction barrier. Mar Drugs. 2014;2(11):5677–97.
Lee EJ, Lim KH. Polyelectrolyte complexes of chitosan self-assembled with fucoidan: an optimum condition to prepare their nanoparticles and their characteristics. Korean J Chem Eng. 2014;31(4):664–75.
Ishihara M, Kishimoto S, Nakamura S, Sato Y, Hattori H. Polyelectrolyte complexes of natural polymers and their biomedical applications. Polymers. 2019;11(4):672.
Mndlovu H, du Toit LC, Kumar P, Choonara YE, Marimuthu T, Kondiah PP, Pillay V. Bioplatform fabrication approaches affecting chitosan-based inter polymer complex properties and performance as wound dressings. Molecules. 2020;25(1):222.
Stenken JA, Poschenrieder AJ. Bioanalytical chemistry of cytokines: a review. Anal Chim acta. 2015;853:95–115.
Liu Y, Yao W, Wang S, Geng D, Zheng Q, Chen A. Preparation and characterization of fucoidan-chitosan nanospheres by the sonification method. J Nanosci Nanotechnol. 2014;14(5):3844–9.
Howling GI, Dettmar PW, Goddard PA, Hampson FC, Dornish M, Wood EJ. The effect of chitin and chitosan on the proliferation of human skin fibroblasts and keratinocytes in vitro. Biomaterials. 2001;22(22):2959–66.
Kingkaew J, Jatupaiboon N, Sanchavanakit N, Pavasant P, Phisalaphong M. Biocompatibility and growth of human keratinocytes and fibroblasts on biosynthesized cellulose–chitosan film. J Biomater Sci Polym Ed. 2010;21(8–9):1009–21.
Senni K, Gueniche F, Foucault-Bertaud A, Igondjo-Tchen S, Fioretti F, Colliec-Jouault S, Durand P, Guezennec J, Godeau G, Letourneur D. Fucoidan a sulfated polysaccharide from brown algae is a potent modulator of connective tissue proteolysis. Arch Biochem Biophys. 2006;445(1):56–64.
Kawano Y, Patrulea V, Sublet E, Borchard G, Iyoda T, Kageyama R, Morita A, Seino S, Yoshida H, Jordan O, Hanawa T. Wound healing promotion by hyaluronic acid: effect of molecular weight on gene expression and in vivo wound closure. Pharmaceuticals. 2021;14(4):301.
Akbarzadeh S, McKenzie MB, Rahman MM, Cleland H. Allogeneic platelet-rich plasma: is it safe and effective for wound repair? Eur Surg Res. 2021;62(1):1–9.
Liu Z, Xiao S, Tao K, Li H, Jin W, Wei Z, Wang D, Deng C. Synergistic effects of human platelet-rich plasma combined with adipose-derived stem cells on healing in a mouse pressure injury model. Stem Cells Int. 2019;2019:3091619.
Sánchez-González DJ, Méndez-Bolaina E, Trejo-Bahena NI. Platelet-rich plasma peptides: key for regeneration. Int J Pept. 2012;2012.
Tohidnezhad M, Bayer A, Rasuo B, Hock JV, Kweider N, Fragoulis A, Sönmez TT, Jahr H, Pufe T, Lippross S. Platelet-released growth factors modulate the secretion of cytokines in synoviocytes under inflammatory joint disease. Mediators Inflamm. 2017;(2017).
Berlanga-Acosta J, Fernández-Montequín J, Valdés-Pérez C, Savigne-Gutiérrez W, Mendoza-Marí Y, García-Ojalvo A, Falcón‐Cama V, Garcia del Barco-Herrera D, Fernández-Mayola M, Pérez-Saad H, Pimentel-Vázquez E. Diabetic foot ulcers and epidermal growth factor: revisiting the local delivery route for a successful outcome. BioMed Res Int. 2017;2017.
Ehrlich HP, Hunt TK. Collagen organization critical role in wound contraction. Adv Wound Care. 2012;1(1):3–9.
Prabhu V, Rao BS, Rao AC, Prasad K, Mahato KK. Photo biomodulation invigorating collagen deposition, proliferating cell nuclear antigen and Ki67 expression during dermal wound repair in mice. Lasers Med Sci. 2020.
Schmidt M, Gutknecht D, Simon JC, Schulz JN, Eckes B, Anderegg U, Saalbach A. Controlling the balance of fibroblast proliferation and differentiation: impact of Thy-1. J Investig Dermatol. 2015;135(7):1893–902.
Patel GK, Wilson CH, Harding KG, Finlay AY, Bowden PE. Numerous keratinocyte subtypes involved in wound re-epithelialization. J Investig Dermatol. 2006;126(2):497–502.
Acknowledgements
The authors acknowledge Dr. Mohamed Hafeezulla Shariff, Pathology Department, Yenepoya Medical College, for help in the PRP preparation and hematological studies.
Funding
The authors received the funding support from DST- SERB, Govt. of India (EMR/2016/0033113). Sneha S. Rao received the ICMR-SRF fellowship (45/54/2020-Nan/BMS).
Author information
Authors and Affiliations
Contributions
Dr. Rekha Punchappady-Devasya: conceptualization, project administration, investigation, manuscript drafting reviewing and editing. Sneha Subramanya Rao: formal analysis, methodology, data curation, validation and manuscript drafting. Dr. Jayachandran Venkatesan: formal analysis, methodology, data curation, validation and manuscript reviewing and editing. Yuvarajan Subramaniyan: methodology (in vivo experiments).
Corresponding author
Ethics declarations
Ethics approval and consent to participate
All the procedures in this study involving human participants were approved by the institutional ethics committee (YEC-1/2019/179), Yenepoya (Deemed to be University). Prior informed consent was obtained from the participants before the collection of blood sample. Similarly, all the procedures involving the animal experiments were approved by the institutional animal ethics committee (YU/IAEC/6/2019), Yenepoya (Deemed to be University).
Consent for publication
All the participants have consented to use the data in the scientific publication without participant identifiers.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Highlights
• Chitosan-fucoidan polyelectrolyte complex (CF) synthesized showed excellent protein encapsulation efficiency with platelet-rich plasma (PRP).
• PRP-loaded chitosan-fucoidan polyelectrolyte complex (CF/PRP) supports sustained release of the proteins.
• The CF/PRP complex enhanced the fibroblast and keratinocyte cell proliferation and migration in vitro.
• Diabetic C57BL/6 mice treated with CF/PRP showed enhanced wound contraction facilitated by cell proliferation and collagen and cytokeratin deposition.
Rights and permissions
About this article
Cite this article
Rao, S.S., Venkatesan, J., Yuvarajan, S. et al. Self-assembled polyelectrolyte complexes of chitosan and fucoidan for sustained growth factor release from PRP enhance proliferation and collagen deposition in diabetic mice. Drug Deliv. and Transl. Res. 12, 2838–2855 (2022). https://doi.org/10.1007/s13346-022-01144-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13346-022-01144-3